Valuable ways to ensure patient adherence in healthcare
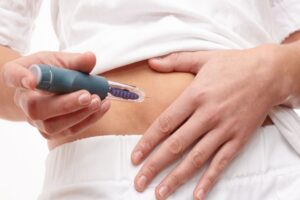
About 50% of people don’t take their drugs exactly as directed. We’re talking about many individuals whose health could be jeopardized if they don’t take their prescriptions as prescribed in terms of timing, dose, and frequency. Unfortunately, there is no “one size fits all” approach to increasing patient adherence to medicine. Every patient is unique, and every situation is unique.
As a result, approaches to what some have dubbed the “sixth vital sign” must also differ. Providers can choose the best intervention method for each patient by determining the root causes of patient noncompliance. Here are some valuable ways to ensure patient adherence in healthcare.
Personalized interventions
A transparent, no-blame strategy like the Momentum patient adherence promotes patient engagement and gives them a forum to voice their treatment-related worries. This enables Healthcare providers to comprehend and foresee any circumstances preventing patients from taking their medication. A plan that works for one patient might not be as successful for another; therefore, it is wise to evaluate each situation individually. The more specifically tailored the solutions are to the patients and their unique challenges, the better.
Ownership of treatment
Patients might feel more in control of their therapy and be more motivated to comply by receiving comprehensive information about it. Patients incentivized to follow will be likelier to do sothan patients who are only passive counsel recipients. This time investment is valuable since knowledgeable and empowered patients are likelier to adhere to their pharmaceutical regimen or device treatment plan.
Similarly, HCPs can determine how active their patients want to be in decision-making by including them in prescribing decisions and tailoring consultation styles to the individual. Patients may need assistance utilizing adherence measures, such as setting up reminder apps or phone alarms.
Interaction, patience, and empathy
Non-adherence should not be viewed as the patient’s fault; patient and HCP collaboration is important for successful adherence. Getting enough support from HCPs is crucial, especially in the early stages of starting a new treatment. HCPs should ensure that all information is available and that patients may make educated decisions regarding their care.
It is beneficial to give clear and comprehensive information regarding the advantages and drawbacks of treatments and medical equipment that are currently accessible, including alternatives to the chosen therapy or gadget. Setting expectations for side effects and the rate of improvement and explaining the justification for treatment choice—such as reduced symptoms—is essential. Last but not least, the patient should be informed of any changes that may be necessary early on so that they are not caught off guard.
Follow-ups
Regular follow-ups should be conducted after the delivery of the initial advice and medication. Teleconsultation makes this easier to accomplish, especially for patients who have grown acclimated to it due to remote working. When it is acceptable, HCPs might advise patients to keep a treatment journal to record their symptoms and any adverse effects. Catch-up appointments give patients the chance to reflect on their experiences and HCPs the opportunity to, if necessary, customize the therapy.
The takeaway
A coordinated strategy, in which patients receive help from organizations and healthcare experts, is optimal for making the tactics above effective